
What Does Psoriasis Look Like
One of the best ways to look nice is to have healthy looking skin, both for men and women. However, the skin is susceptible to all sorts of conditions that can leave noticeable marks, from simple pimples to more serious skin conditions. One of the latter types is psoriasis.
Related Topics (Sponsored Ads):
Psoriasis is a chronic autoimmune condition that affects the skin, causing it to develop red, scaly patches. This condition is characterized by an overactive immune system that speeds up the growth cycle of skin cells, leading to the rapid accumulation of cells on the skin’s surface. Understanding the visible symptoms of psoriasis, its diagnosis, and management is crucial for individuals affected by this condition.
Overview
Psoriasis is a non-contagious, inflammatory skin condition that affects approximately 2-3% of the global population. It can occur at any age, but it most commonly appears between the ages of 15 and 35. The severity of psoriasis can vary from mild, with small patches of scaly skin, to severe, with widespread plaques covering large areas of the body. Psoriasis can also affect the nails, scalp, and joints, leading to discomfort and reduced quality of life for those affected.
Visible Symptoms of Psoriasis
This condition has distinct visible symptoms that can vary in appearance and severity. The most common visible symptoms include:
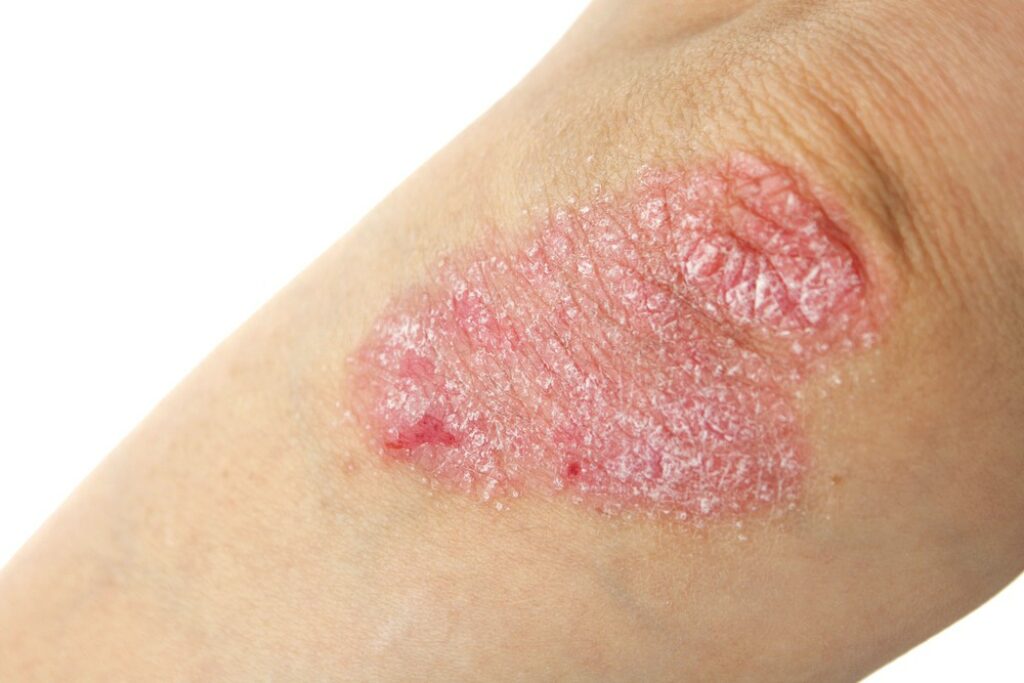
-Red Patches of Skin: Main symptom often manifests as raised, inflamed patches of red skin, known as plaques. These plaques can appear anywhere on the body, including the elbows, knees, scalp, and lower back.
– Silver-White Scales: Over the red patches of skin, silvery-white scales develop, creating a characteristic appearance that distinguishes psoriasis from other skin conditions.
-Itching and Discomfort: The affected areas may itch and feel sore or tender, leading to discomfort and irritation.
– Nail Changes: Psoriasis can cause pitting, discoloration, and thickening of the nails, leading to nail abnormalities.
– Scalp Psoriasis: In some cases, it affects the scalp, resulting in red, scaly patches or significant flaking of the skin.
– Joint Pain and Swelling: Psoriatic arthritis is a specific form of arthritis that affects some individuals with psoriasis, leading to joint pain, stiffness, and swelling.
What Not to Confuse Psoriasis With
It is important not to confuse psoriasis with other skin conditions that may appear similar but require different treatment approaches. Conditions that may resemble psoriasis include:
Eczema: While eczema (atopic dermatitis) can also cause red, inflamed skin patches, it typically presents with a different texture and appearance. Eczema patches are often more moist and oozing, whereas psoriasis plaques are characterized by silver-white scales.
Ringworm: Ringworm is a fungal infection that can cause red, circular patches on the skin. Unlike psoriasis, ringworm is contagious and requires antifungal treatment.
Seborrheic Dermatitis: This condition can resemble scalp psoriasis but is caused by a different underlying mechanism. Seborrheic dermatitis often leads to flaky, greasy, and yellowish scales on the scalp.
Allergic Reactions: Allergic reactions, such as contact dermatitis, can cause red, inflamed skin patches due to exposure to irritants or allergens. However, these reactions typically subside once the trigger is removed, unlike the persistent nature of psoriasis.
Diagnosing Psoriasis
Diagnosing psoriasis involves a thorough examination by a dermatologist or healthcare professional. In some cases, a skin biopsy may be necessary to confirm the diagnosis. The following diagnostic methods may be used:
Physical Examination: The healthcare provider will examine the skin and nails to assess the appearance of the lesions and determine if they align with the typical characteristics of psoriasis.
Medical History: Providing a detailed medical history, including family history of psoriasis or other autoimmune conditions, can aid in the diagnosis.
Skin Biopsy: In some cases, a small sample of skin tissue may be removed and examined under a microscope to confirm the diagnosis of psoriasis and rule out other skin conditions.
Self-Help Tips to Manage Psoriasis Symptoms
While there is no cure for psoriasis, several self-help tips can help manage the symptoms and improve the overall quality of life for individuals affected by this condition:
Moisturize Regularly: Keeping the skin well-hydrated can help reduce the itching and scaling associated with psoriasis. Use fragrance-free moisturizers and apply them after bathing or showering.
Avoid Triggers: Identify and avoid triggers that exacerbate psoriasis symptoms, such as stress, certain medications, alcohol, and smoking.
Gentle Bathing: Take short, lukewarm baths using mild, non-irritating soaps. Avoid hot water and harsh scrubbing, as these can worsen psoriasis symptoms.
Sunlight Exposure: Some individuals find that regular, short periods of sun exposure can help improve their psoriasis symptoms. However, it is essential to protect the skin from excessive sun exposure and use sunscreen.
Stress Management: Stress is known to trigger or worsen psoriasis symptoms. Engage in stress-reducing activities such as yoga, meditation, or deep breathing exercises.
Healthy Diet: Eating a balanced diet rich in fruits, vegetables, lean proteins, and whole grains can support overall health and potentially improve psoriasis symptoms.
Seek Support: Joining support groups or seeking counseling can provide emotional support and valuable tips for managing the challenges of living with psoriasis.
Conclusion
Understanding the visible symptoms of psoriasis, its diagnosis, and management is important for individuals living with this chronic skin condition. By recognizing the distinct appearance of psoriasis, seeking an accurate diagnosis, and implementing self-help strategies, individuals can effectively manage their symptoms and improve their overall well-being. While psoriasis presents unique challenges, a proactive approach to self-care and seeking professional guidance can significantly improve the management of this condition.




